

For a dentist, treating a patient’s healthy but unsightly teeth has proven to be very difficult. One of the most aesthetically pleasing ways to have a more beautiful and pleasing smile is with porcelain laminate veneers. The location, shape, size, and color of teeth can all be changed using porcelain veneers. They only need a small amount of surface enamel reduction (0.5–0.7 mm) to prepare the teeth. The primary subject of this study is a patient who had repeated restorations done on an anterior region with composite. The patient received porcelain laminate veneers for aesthetic correction in the maxillary anterior region with good cosmetic results, which lends credence to the notion that minimally invasive porcelain laminate veneers could become a conservative and adaptable ally in the aesthetic dentistry domain.
Key words: Aesthetics, Porcelain laminate veneers, Composite restoration.
A confident smile is the most beautiful
accessory somebody can have. A self-assured
smile is an essential aspect of each person’s personality. People are starting to place a higher
importance on having a gorgeous, healthy
smile. Cosmetic dentistry has developed, giving
dentists additional options for conservative and
aesthetically acceptable repair techniques1,2.
There has always been difficulty in restoring
unsightly anterior teeth because it involves a lot
of healthy tooth tissue and has a negative impact
on the pulp and gingiva. A more conservative
option for enhancing the appearance of anterior
teeth than full coverage restorations are laminate
veneers. The available treatments that restore
and optimize the appearance of anterior teeth
are the least intrusive ones.
In order to enhance a tooth’s appearance,
extremely thin porcelain shells known
as porcelain veneers or dental porcelain
laminates are luted to the front of teeth.
A thin porcelain shell is securely attached to a
tooth using its bonding power of material. When
porcelain is effectively bonded to a tooth, its
naturally fragile nature transforms into one of
extreme robustness and durability3.
Veneers are a dentist’s suggested and frequently
requested treatment due to their mechanical,
aesthetic, and biocompatible properties, as well as their ability to preserve tooth structure,
last a long time, be dependable, and improve
bonding strength4. This article covers a case
where porcelain laminate veneers were used
conservatively to correct a stained anterior
restoration in order to attain the desired cosmetic
results.
OUTLINE OF THE CASE
Diagnosis
A female patient, age 24, came to the
prosthodontics department to have her
upper anterior teeth restored in an aesthetic
manner. Her goal was long-term repair, with
better aesthetics being her main priority. The
results of the clinical evaluation showed that
the left and right central incisors were cracked
at the incisal area, and composite was used
to reconstruct them. The patient’s past dental
history indicated that the discoloration of the
aesthetic restoration caused the central incisors
to undergo repeated procedures over the course
of four years.
Every standard clinical and radiological
examination fell well within acceptable bounds.
An overbite of 3 mm and an overjet of 2 mm
were noted during the intraoral examination.
When the patient initially arrived, they had a
good periodontal state, a thin gingival biotype,
a medium frenal attachment (Class II), and
adequate dental hygiene.
The patient was given information on a number
of treatment options, including laminates, a full
crown, and a repeat of a composite restoration.
After being informed of the benefits and
drawbacks of each therapy, the patient decided
to have porcelain laminate veneers (PLV).
Treatment plan
A comprehensive case history, clinical
assessment, radiological analysis, and any additional required research were completed.
The cost aspect was also assessed. The treatment
approach chosen was a modest tooth preparation
for laminate with quick provisionalization.
Procedure
Prior to undertaking any interventional
procedures, a thorough oral prophylaxis was
completed to ensure optimal periodontal health.
Subsequent diagnostic evaluation included
radiographic imaging to assess the underlying
structures. Based on clinical and radiographic
findings, the treatment plan for the maxillary
right and left incisors involved the incorporation
of an incisal overlap design with a proximal
wraparound extension to enhance retention,
stability, and functional integration.
First, the Veneer depth cutting (LVS1) bur was
used to place the labial surface’s initial depth
orientation grooves. Using a long, round-end
tapered standard grit diamond bur, a chamfer
finish and 0.5 mm labial reduction were obtained
with a sulcular extension of 0.2–0.3 mm. The
contact region was located 0.2 mm labial to
the mesial and distal finish lines. A gingivally
sloping 1 mm incisal reduction from the labial
was carried out. A rounded chamfer was created
in the lingual enamel down to a depth of 0.5–1
mm. To reduce postoperative sensitivity and to
achieve good bonding, the overall reduction was
limited to the enamel.

Gingival retraction was achieved by impregnating
a retraction cord (Ultrapak Dental retraction
cord #00) with hemostatic gel (Hemostal GelTM,
Prevest DenPro, USA) for a duration of two minutes
(Fig:1). Making use of vinyl polysiloxane (Photosil
TM, India, DPI) Final impressions were made in
a custom tray and submitted to the laboratory
after a two-stage putty wash procedure (Fig:2).
choose a shade. Provisionals were created using
composite because the preparation was in an
aesthetic area.

Using the heat press method, veneers were
created from lithium disilicate material (IPS
e.max Press, Ivoclar Vivadent, Lichtenstein).
After the laminate veneers were received from the
laboratory, a few days later a clinical try-in was
conducted to assess the protruding interferences,
contacts, color match, shape, and marginal fit.
Following verification of proper clinical seating
and confirmation of the absence of occlusal
interferences along the lingual surfaces, the
veneers were deemed clinically acceptable and
subsequently approved for definitive bonding.
On the day of cementation, two days following the
try-in, the veneers’ intaglio surface was etched
using Ivoclean or 5% hydrofluoric acid (IPS
Ceramic Etching Gel, Ivoclar Vivadent AG) for 20
seconds. Following cleaning and drying, silane
coupling agent (Ivoclar Vivadent, Monobond®
N) was used. After etching the prepared tooth
surfaces for 15 seconds with 35% phosphoric acid
(ScotchbondTM, 3M ESPE), the surfaces were
washed with pumice slurry, rinsed with water,
and left to air dry. Subsequently, a bonding agent
was meticulously applied to the prepared tooth
surfaces in accordance with the manufacturer’s
recommendations, ensuring optimal adhesion
for the planned restorative procedure. (Single
Bond Universal Adhesive, 3M ESPE).
Using an adhesive tip applicator, a light cure
resin luting agent of transparent shade (RelyXTM
Veneer cement, 3M ESPE) was applied to the
porcelain veneers’ intaglio surface and then
carefully set on the teeth. Following a five-second
tack-curing phase, the restoration margins
were carefully evaluated to ensure complete
seating and proper adaptation to the prepared
tooth structure. After removing extra luting
cement, each tooth underwent light curing for 30
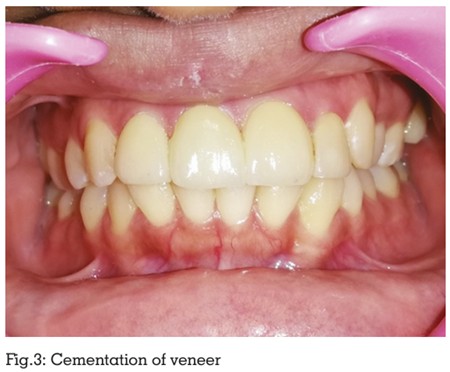
seconds to ensure full polymerization. Occlusal interferences were carefully evaluated following
veneer placement (Fig:3). Proximal contacts
were assessed using dental floss to verify proper
contact integrity, and the results were deemed
clinically satisfactory. (Fig:4). To optimize the
long-term success of the restorations, the patient
was advised to maintain rigorous oral hygiene
measures, avoid direct incisal loading on hard foods, and comply with a structured recall
regimen at one week, one month, six months,
and annually for continued monitoring and
maintenance. (Fig:5)

Research indicates that porcelain veneers are
a good conservative and aesthetically pleasing
treatment choice. The advantages of employing
these restorations include their strong resistance
against abrasion, stability, reduced chance
of generating irritation or sensitivity, less
cytotoxicity, and biological acceptability to
the body due to their higher chemical stability.
Additionally, they take a cautious stance and
refrain from removing too much natural teeth4.
Owing to their uniformly glazed surface, these
restorations show less plaque accumulation and
easier cleaning. The thinness of the ceramic (0.3
0.5mm) makes the veneers brittle even before
they are glued. However, once attached to the
scratched enamel surface, they become more
robust and blend in with the tooth structure.
Nevertheless, they do have certain drawbacks.
Porcelain laminate veneers cannot be applied
to areas with extreme crowding, loss of enamel,
or parafunctional habits. For teeth with dark
stains, veneers are not the ideal repair. When
veneers are used to treat worn-down teeth with
considerable dentin exposure, improper bonding
onto pre-existing composite restorations can
lead to veneer failure. The tendency of heat
fluctuations to produce veneer cracking when
the porcelain is thin and the luting composite is
thick is another risk factor. When the ceramic and
luting composite thickness ratios are not larger
than three to one, the least degree of cracking is
observed.
The patient’s selection is crucial to the
effectiveness of porcelain veneers. in present
case the patient’s young age and their inclination
towards wear, slight fractures, and discoloration, the lifespan of the composite materials used in
this case is dubious5,6. In this case, porcelain
laminate veneers were the best course of action
because the patient had a normal overjet and
overbite, a nice smile line, no parafunction,
and sufficient enamel. Modern prosthodontics
has undergone a paradigm change to support
the growing interest in using conservative
restorative options. The provision of minimally
invasive dentistry has been under more scrutiny
and demand in recent literature in order to give
excellent care with the least amount of tooth
structure removed. In order to improve strong
bonding, retention, aesthetics, and strength, it
has thus been considered a workable strategy to
preserve the patient’s tooth structure7,8.
The literature has described a number of methods
for treating anterior shattered teeth, including
full-contour porcelain crowns, porcelain laminate
veneers, and composite resin restorations. The
biggest disadvantage of composite restorative
materials is that they require numerous follow
ups and become stained with time, despite being less expensive and time-consuming. Laminated
veneers are a more cautious alternative.