


Introduction
The evolution of prosthodontics is increasingly shaped
by technological advances. With the rise of digital
tools, the traditional foundation of analog techniques is
being re-evaluated. A significant academic and clinical
question arises: Should training and practice prioritize
digital workflows from the start (“Digital First”), or should
they be built on traditional foundational skills first
(“Fundamentals First”)? This article explores the clinical,
educational, and philosophical implications of each
approach and proposes a balanced, integrative model
supported by academic evidence and comparative data.
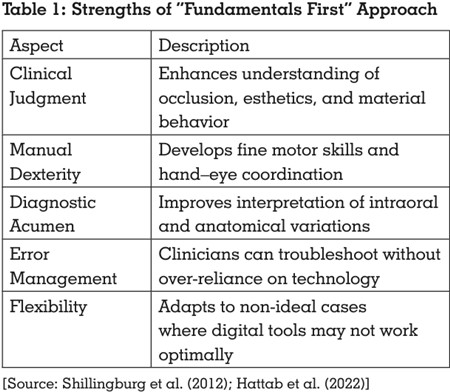
Understanding the Fundamentals of Prosthodontics
Historically, prosthodontics has been centered on the
mastery of basic techniques: accurate impressions,
occlusal harmony, articulation, esthetic evaluation, and
manual dexterity. These fundamentals are taught using
conventional tools like facebows, articulators, and wax
ups. They are not merely technical steps; they cultivate
critical thinking, clinical judgment, and anatomical
understanding.
Digital Dentistry: A Transformational Shift
Modern prosthodontics now incorporates CAD/CAM
systems, 3D printing, intraoral scanners, and virtual
smile design. These innovations offer unprecedented
levels of efficiency, accuracy, and patient engagement.

Education: The Crossroads of Two Eras
In prosthodontic education, the sequencing of digital
and analog training impacts how students develop
critical competencies. There is debate over whether
digital methods hinder or help the formation of deep
understanding in early learners.

Clinical Application and Workflow Flexibility
In practice, clinical decision-making benefits from both
analog and digital expertise. For instance, full-arch
implant prostheses may benefit from digital planning and guided surgery but still require foundational
knowledge to assess occlusal schemes and esthetic
zones.
Moreover, the accuracy of intraoral scanners in
edentulous cases, long-span arches, or deep subgingival
margins can still be questionable (Mangano et al., 2016).
In such cases, analog impressions provide a safety net.
A clinician grounded in fundamentals can identify when
digital systems produce errors, whether from motion
artifacts, scan stitching errors, or soft tissue collapse.
Thus, digital workflows do not replace fundamentals but
rather depend on them for effective implementation.
Professional Identity and Future Skillsets
As technology advances, the role of the prosthodontist
evolves from being a hands-on craftsman to a digital
coordinator—designing prostheses, interpreting 3D
images, and supervising milling or printing. This shift
demands new competencies but must not come at the
expense of foundational knowledge.
The modern prosthodontist should be both a diagnostician
and a digital artisan. Understanding tooth morphology,
occlusal dynamics, and esthetics allows clinicians to
evaluate software-generated designs critically. Without
these insights, a prosthodontist becomes a technician
rather than a clinician.
The American College of Prosthodontists (2022)
emphasizes this integration in their competency
statements, advocating that students demonstrate
proficiency in both digital and conventional methods.
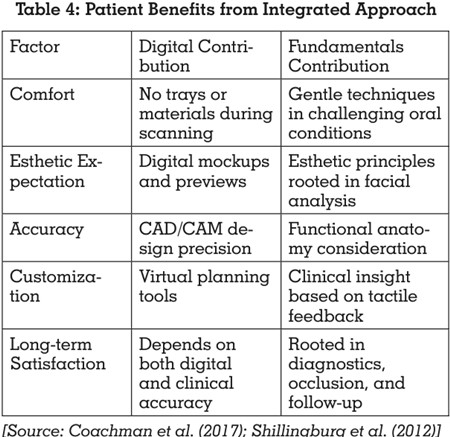
Patient-Centered Outcomes: A Unified Priority
While digital tools offer a more engaging and comfortable
experience, the success of any prosthodontic procedure
depends on sound diagnosis and customization.
Towards a Synthesis: Integrative Prosthodontics
Rather than viewing “Digital First” and “Fundamentals
First” as opposing philosophies, the future lies in
integration. Curricula should be restructured to teach
both in tandem, allowing students to develop manual
skills while engaging with digital tools contextually.
The goal is not to choose between tradition and
innovation but to blend them—leveraging technology to
enhance, not replace, foundational expertise.
Faculty training, infrastructure investment, and
pedagogical redesign are critical to achieving this
balance. Institutions should provide access to intraoral
scanners, 3D printers, and virtual planning software
while continuing to emphasize clinical reasoning,
occlusion analysis, and treatment planning.
Conclusion
In prosthodontics, both digital technologies and
foundational principles are essential. Digital tools offer
speed, precision, and enhanced patient engagement,
while fundamentals provide depth, adaptability, and
diagnostic accuracy. The best prosthodontists will be
those who master both realms—those who can scan and
mill, but also assess esthetics, manage occlusion, and
adapt designs based on clinical realities.
The future of prosthodontics does not lie in choosing
between “Digital First” and “Fundamentals First” but in
strategic integration. The optimal approach combines
early exposure to digital tools with a solid grounding
in foundational prosthodontic concepts. This balanced
philosophy supports deeper learning, clinical flexibility,
and better patient outcomes.
As the profession transitions, educators, institutions, and
clinicians must collaborate to redesign curricula and
clinical protocols that empower future prosthodontists to
be both digitally fluent and clinically wise.
References